Abstract
Introduction:
Daratumumab (Dara) is an anti-CD38 monoclonal antibody representing a novel treatment agent for multiple myeloma (MM). Nonetheless, several studies have reported a Dara-related impairment of CD34+ hematopoietic stem cell (HSC) mobilization and post-autologous stem cell transplantation (ASCT) complications, including low yields of mobilized HSCs and delayed neutrophil engraftment. Impact of Dara on the mobilization process and HSCs remains poorly understood even though sufficient yields of CD34+ cells are necessary for a successful ASCT and subsequent patient recovery.
Aims:
To compare the effect of the Dara-containing (Dara-Bortezomib-Dexamethasone [D-VCd]) and conventional (Bortezomib-Thalidomide-Dexamethasone [VTd]) therapy on CD34+ HSCs.
Methods:
Transplant eligible MM patients were treated with D-VCd or VTd induction regimen followed by a cyclophosphamide + G-CSF mobilization and a high-dose melphalan D -1 before ASCT. Flow cytometry (FCM) screening of CD34+ subsets was performed in the bone marrow (BM) or apheresis product (AP) at three consecutive time points: 1) diagnostic BM (DG), 2) mobilization AP (MOB), 3) a day prior ASCT BM (D-1). Furthermore, RNA sequencing (RNAseq) of sorted CD34+ cells was performed on total RNA with ribo-depletion protocol in AP after the induction. D-VCd samples had lower RNA yields thus the D-VCd or VTd groups were processed as independent batches.
Results:
Clinical data revealed no significant differences in mobilization (p >0.050) likely due to a small cohort sizes (D-VCd n=5 vs VTd n=9), though a trend towards worse performance in D-VCd was observed. Median CD34+ cell yield was 3.08 vs 10.56 x 10 6/kg. Platelet recovery of >20x10 9/L was D+14 vs D+12 (range: 11-18 vs 10-16). Neutrophil recovery of >0.5x10 9/L was D+12 in both groups (range: 11-17 vs 11-12).
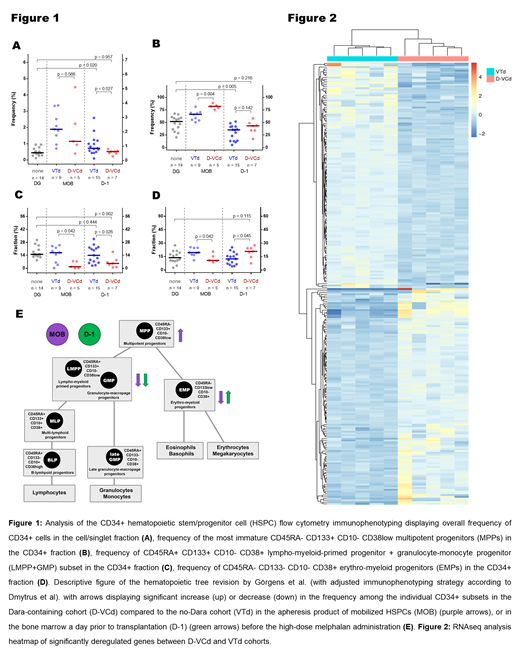
In FCM analysis, DG (n=14), MOB D-VCd (n=5) vs VTd (n=9), D-1 D-VCd (n=7) vs VTd (n=15) were compared. CD34+ frequency (Fig. 1A) difference in MOB D-VCd vs VTd was insignificant (median: 1.15% vs 1.89%), whereas CD34+ fraction dropped in D-1 D-VCd (median: 0.52% vs 0.72%, p=0.027), albeit there was no significant reduction in D-1 D-VCd vs initial DG (median: 0.52% vs 0.45%). Differences in the distribution of certain HSC subsets were detected in the CD34+ pool (Fig. 1B-E). Frequency of multipotent progenitors (MPPs) (Fig. 1B) was increased in MOB D-VCd (median: 82.1% vs 66.2%, p=0.004). Frequency of lympho-myeloid-primed progenitor + granulocyte-monocyte progenitor (LMPP+GMP) (Fig. 1C) subset was reduced in D-VCd in both MOB (median: 1.7% vs 16.9%, p=0.042) and D-1 (median: 5.3% vs 14.0%; p=0.026). Erythro-myeloid progenitors (EMPs) (Fig. 1D) were reduced in MOB D-VCd (median: 10.7% vs 19.5%, p=0.042), while the frequency of EMPs increased in D-1 D-VCd (median: 20.8% vs 12.4%, p=0.045). No considerable differences were found in the expression of adhesion molecules CD44/HCAM or CD184/CXCR4. CD38 was strongly diminished in the whole D-VCd CD34+ fraction of MOB and D-1.
To understand whether the differences in the mobilization efficacy after D-VCd induction were reflected in the expression profile of mobilized CD34+ cells, differential expression analysis was performed. Overall 133 significantly deregulated genes (p<0.05; log fold change >(-)1) between cohorts (D-VCd n=5 vs VTd n=5) were revealed (Fig. 2). Pathway analysis showed cellular response and localization as the most deregulated categories. The list of deregulated genes contained 25% of non-coding RNAs, some of which were linked to a protein localization in the cell (RN7SL1/2). The expression of adhesion molecules was inspected independently. Out of 59 HSC hallmark genes, only 8 were significantly altered in D-VCd. Interestingly, the main homing molecule CXCR4 seemed to be downregulated in D-VCd, while integrins A3 and B4 were upregulated.
Conclusions:
Despite the limited cohort sizes, a prospective trend of delayed neutrophil and platelet recovery was observed after D-VCd therapy. FCM analysis revealed a significant reduction of CD34+ subsets responsible, among others, for a reconstitution of neutrophils and megakaryocytes. A strong signal in transcriptome data which would potentially explain differential mobilization in D-VCd cohort was not detected, nevertheless, several genes with adhesive/homing and stem cell differentiation function were indeed altered. The results warrant further investigation.
Hajek: BMS: Consultancy, Honoraria, Research Funding; AbbVie: Consultancy, Honoraria; Novartis: Consultancy, Research Funding; Janssen: Consultancy, Honoraria, Research Funding; Amgen: Consultancy, Honoraria, Membership on an entity's Board of Directors or advisory committees, Research Funding; Pharma MAR: Consultancy, Honoraria; Celgene: Consultancy, Honoraria, Research Funding; Takeda: Consultancy, Honoraria, Membership on an entity's Board of Directors or advisory committees, Research Funding.